
Researchers identify a new culprit behind fibrosis
Published Date
By:
- Liezel Labios
Share This:
Article Content
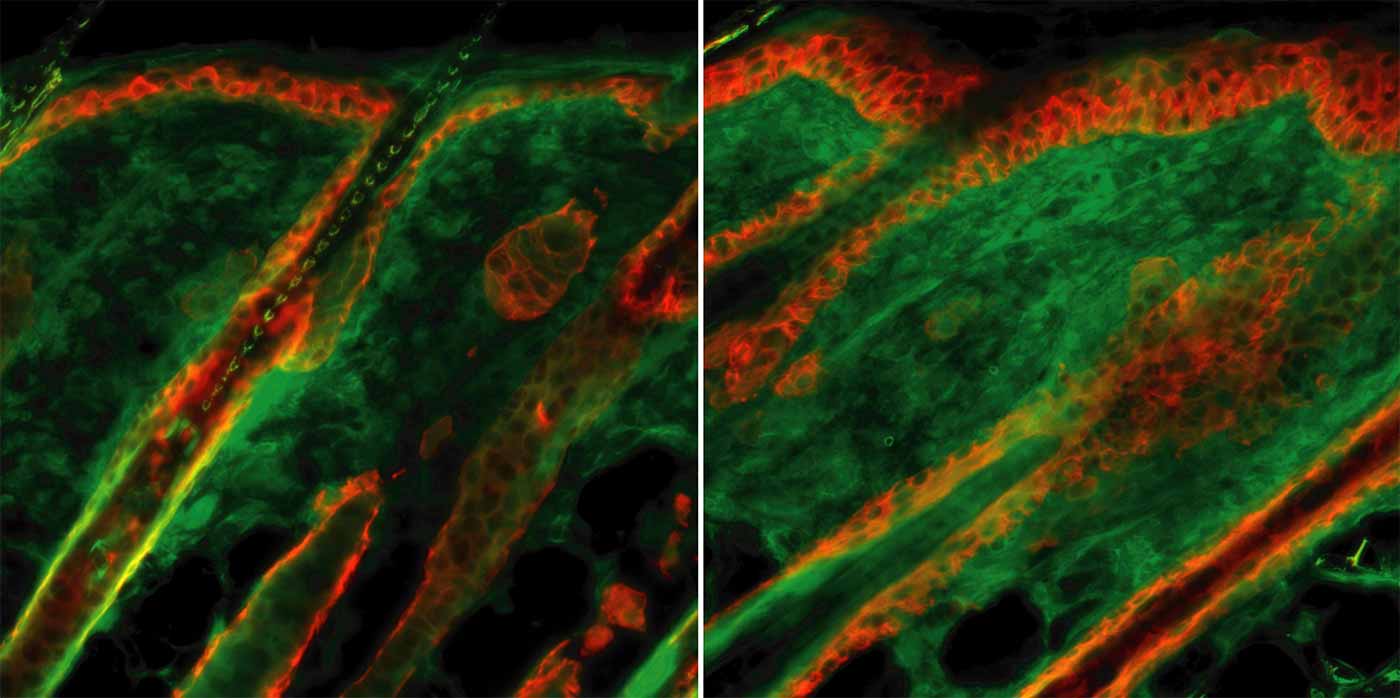
Images of skin sections from wild-type mice (left) and mice genetically engineered to develop skin fibrosis (right). The skin sections were stained for elastin (green), which is present in much higher levels in the fibrotic skin tissues, and keratin (red).
An international team of researchers has identified a new molecule involved in skin fibrosis, a life-threatening disease characterized by the inflammation and hardening of skin tissue. The new study is the first to investigate the role of this molecule in skin fibrosis and paves the way toward new and improved therapies for the disease.
The study reveals a new mechanism for the development of fibrosis in skin tissues and could potentially be relevant to other organs that develop fibrosis such as the lungs, heart, liver and kidney, said researchers. The team, led by bioengineering professor Shyni Varghese at the University of California, San Diego and Colin Jamora, a biologist at the IFOM-inSTEM Joint Research Laboratory in India, published the findings in the Oct. 15 issue of Nature Communications.
“We’ve identified a new component that hasn’t previously been studied as a factor contributing to fibrosis,” said Varghese. “This discovery gives us a new understanding of how fibrosis forms and could help us develop therapeutic strategies that are more effective than existing ones.”
Fibrosis is a condition in which tough, fibrous connective tissues develop in an organ, similar to scar tissues that form after injuries. The disease can affect various tissues, including those of the skin, lungs, heart and liver. Due to the development of tough, fibrous matter, fibrosis causes the affected tissues to stiffen, swell, and eventually lose their normal functions. The exact mechanism by which fibrosis develops is not yet clearly understood, and there are no proven cures or treatments for the disease.
In this study, researchers discovered that a molecule called fibulin-5 played a role in the development of skin fibrosis in mice. Fibulin-5 is responsible for the formation of elastin, a protein that enables skin to bounce back to its original shape after being stretched. Elastin is a small component of connective tissues in the body, and little is known about its contribution to fibrosis.
Since a large component of connective tissue is made of collagen, most research on the underlying cause of fibrosis has so far focused on the overproduction of collagen. However, the role of less abundant proteins like elastin has been largely ignored, until now.
“Clinical trials to test the effectiveness of potential therapies for many known fibrotic diseases have so far been disappointing. Our study points to a new way to target this debilitating disease,” said Jamora.
By focusing on elastin, the team discovered that the development of fibrosis in skin tissues was linked to a particular molecule: fibulin-5. Researchers studied mice that were genetically engineered to develop skin fibrosis and found substantially higher levels of fibulin-5 in their skin tissues than in normal mice. High levels of fibulin-5 were also found in the skin tissues of human patients with skin fibrosis. Researchers explained that elevated levels of fibulin-5 caused elastin to form in abnormally large amounts, and that higher elastin levels likely contributed to increased skin tissue inflammation and stiffening.
Researchers also demonstrated that removing fibulin-5 from the genetically engineered mice before they developed skin fibrosis helped prevent all the symptoms of skin fibrosis — including skin tissue inflammation and stiffening — from occurring.
“Manipulating the fibulin-5 levels could be a therapeutic strategy to treat skin fibrosis,” said Varghese.
“With further studies, we are looking to provide hope for a disease condition that contributes to approximately 30 percent of all deaths worldwide,” said Jamora.
As a next step, researchers are exploring methods to inhibit the increase of fibulin-5 and determine whether fibulin-5 plays a role in fibrosis development in other organs besides the skin. One of their goals is to translate this proof of concept study on mice to clinical trials in the future.
The work was supported by grants from the National Institute of Arthritis and Musculoskeletal and Skin Diseases under the National Institutes of Health (NIH/NIAMS), Scleroderma Foundation, and core funds from inStem and IFOM.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


