
By:
- Jeanna Vazquez
Published Date
By:
- Jeanna Vazquez
Share This:

With the help of their nurses, the two childhood friends reunited while seeking treatment at UC San Diego Health. Note: Because both were current patients at the time and consistently monitored for any infection that could negatively impact their procedures, including COVID-19, they were able to safely visit with each other.
Out of Thin Air
Two childhood friends who suffer from lung disease reunite while seeking treatment at UC San Diego Health
A lifelong athlete, Jillian Queri knew something was terribly wrong one morning while living abroad in Australia when, while surfing, she began struggling to breathe and almost drowned. In a hospital emergency department, Jillian learned she had multiple pulmonary embolisms, or blood clots, in her lungs and deep vein thrombosis (DVT) in her arm.
“I finished the rest of the year in Australia regularly taking blood thinners, but I still wasn’t feeling well, and when I returned to the United States, my condition deteriorated significantly.”
After multiple visits with specialists in her hometown of Park City, Utah, Jillian was diagnosed with Chronic Thromboembolic Pulmonary Hypertension (CTEPH).
CTEPH is caused by repeated or unresolved blood clots in the pulmonary arteries that lead to scarring within the blood vessels of the lungs. Pulmonary embolism is a fairly common, but potentially serious cardiovascular condition that usually resolves with medical therapy, such as blood thinners. In some cases, however, blood clots do not go away or they recur. When this happens, the lungs experience harmful vascular changes that can result in pulmonary hypertension.
One of the leading causes of right-sided heart failure, CTEPH can be deadly if left untreated. It is also relatively rare; there are approximately 12,000 new cases of CTEPH in the United States each year.
“Once I was diagnosed, I began researching the disease,” said Queri. “I ended up on the Pulmonary Hypertension Association website reading patient stories when I saw a face I thought looked super familiar, but couldn’t quite place how I knew him.”
That familiar face ended up being Jillian’s childhood friend, Ian Bartlett, whom she hadn’t seen since the 5th grade, 15 years earlier. Ian had also been diagnosed with CTEPH.
“I was diagnosed with CTEPH in March of 2019 after dealing with multiple DVTs in my shoulders and pulmonary embolisms for more than three years,” said Bartlett. “I’ve always been super active so dealing with this can be extremely frustrating. I ski, play soccer, hike, enjoy going backpacking—everything.”
“I realized something must be really wrong when I was skiing one day and got really out of breath, I couldn’t catch my breath for nearly 10 minutes.”
After his diagnosis, Bartlett began treatment at UC San Diego Health in November of 2019. Queri would soon follow.
Comprehensive treatment plans
UC San Diego Health is a worldwide leader in the diagnosis, treatment and research of pulmonary vascular disorders, including CTEPH and pulmonary embolism. For both Queri and Bartlett, their treatment plans were led by a multidisciplinary team of pulmonologists, cardiologists, surgeons, radiologists, anesthesiologists, respiratory therapists and specialized nurses.
While rare, CTEPH is likely more prevalent than currently recognized because the symptoms—such as shortness of breath, fatigue or discomfort—are nonspecific. Patients are often misdiagnosed with more common conditions, such as asthma or Chronic Obstructive Pulmonary Disease (COPD), leading to substantial delays in appropriate treatment.
“On average these patients will go around two years before someone makes the correct diagnosis,” said Dr. Nick Kim, pulmonologist, section chief of Pulmonary Vascular Medicine at UC San Diego Health. “By the time we meet them, some of our patients are quite late in their disease with signs and symptoms of end-stage, right-sided heart failure from their CTEPH. However, there is no degree of disease severity that we cannot treat. Indeed, such patients with severe cases can exhibit some of the most dramatic responses to our treatment.”
There are two procedural treatment options for CTEPH: Pulmonary Thromboendarterectomy (PTE) and Balloon Pulmonary Angioplasty (BPA).
PTE was pioneered at UC San Diego Health.
Pulmonary Thromboendarterectomy
For Jillian, she was a candidate for PTE, a complex surgical procedure that removes blood clots and scarring from major blood vessels in the lungs to restore blood flow.
To remove the clots, surgeons must see clearly into the lungs’ tiny arteries, which requires operating without any blood present. To achieve this, the patient’s body is cooled using a heart-lung machine. Once body temperature reaches approximately 64 to 68 degrees, blood circulation is stopped and blood volume reduced to create a bloodless surgical field.
“When we perform open-heart surgery, we use the heart-lung machine to stop the heart so we can treat the patient,” said Dr. Michael Madani, chief of Cardiovascular and Thoracic Surgery, and executive director of Cardiovascular Institute-Surgery at UC San Diego Health. “With PTE, we’re taking it one step further by stopping blood flow completely. This process is called circulatory arrest in which we cool the body’s cells and drain the body of blood to a point where circulation momentarily stops.”
During circulatory arrest, surgeons remove clots from the patient’s lung arteries and any scarring. Then they slowly restart the body’s circulation and warm the patient back to normal temperatures.
On average, a PTE procedure will last around 9 to 10 hours.
UC San Diego Health has performed nearly 4,500 PTE procedures, more than any other institution in the world. For the past decade, the program has reported a mortality rate of approximately 1 to 2 percent—the lowest known postoperative mortality rate worldwide.
“Having the largest number of these procedures in the world with the best outcome is a representation of the dedication of our multidisciplinary team and shows what we can accomplish at UC San Diego Health,” said Madani. “I couldn’t be more proud of our team that I’m privileged to be a part of.”
Balloon Pulmonary Angioplasty (BPA)
Some individuals are not candidates for PTE surgery. For them, UC San Diego Health offers Balloon Pulmonary Angioplasty (BPA), plus palliative interventions with targeted medical therapy.
“We take pride in the fact that regardless of what type of CTEPH treatment a patient needs, we can provide them with the right therapy specific for them. We’re the one-stop shop,” said Dr. David Poch, director of Pulmonary Artery Hypertension Medicine at UC San Diego Health. “Our goal is to get our patients back to their normal lives.”
Bartlett was a candidate for BPA because of the location of his blood clots.
BPA is reserved for patients like Barlett in which the clots are too difficult to reach using surgery. The procedure is interventional and performed in the cardiac catheterization lab where interventional cardiologists expand scar tissue caused by blood clots to improve the radius and flow within an artery.
During the procedure, a small catheter is inserted into an artery in the neck or groin. A second hollow tube containing wires and a balloon is then introduced through the catheter and threaded to the diseased lung vessels.
“Through X-ray images, we measure pressures in the patient’s narrowed vessels and guide the wires and balloon to the site of the blood clot or blockage,” said Dr. Ehtisham Mahmud, executive director Cardiovascular Institute-Medicine at UC San Diego Health. “The balloon is then inflated to disrupt the blood clots and we push the blockages into the walls of the arteries. Afterwards, the balloon is deflated and removed through the same catheter.”
Patients receiving BPA need to undergo approximately six to eight treatment sessions to remedy their CTEPH. Mahmud said patients typically experience a noticeable improvement in overall health and ability to breathe after each session.
“In some ways, BPA is a complementary procedure to PTE because it provides another treatment option for our patients so they can get the help they need for their specific form of CTEPH,” said Mahmud.
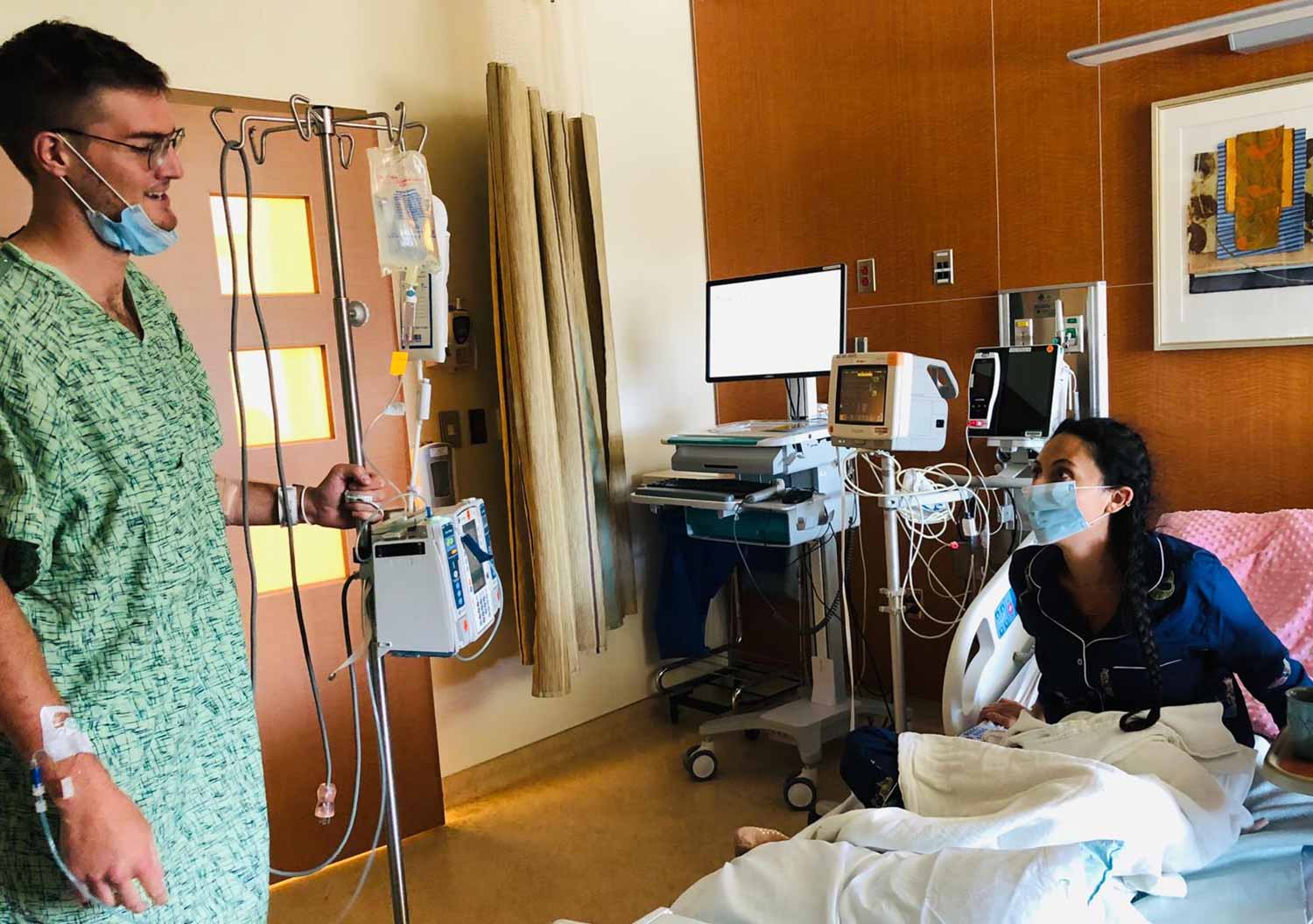
A reunion
On June 11, 2020, Jillian underwent her PTE procedure with Madani at UC San Diego Health. Coincidentally, Ian was recovering from his fourth BPA treatment session with Mahmud.
Both still live in Utah, but this was their closest physical encounter since the 5th grade.
“I’m on social media and I get this message from Jillian asking if I’m at UCSD,” said Bartlett. “I reply saying, ‘Yeah, I’m on the second floor of the hospital’ and she responds saying she’s on the third floor. It was so random!”
“It was such a weird coincidence,” said Queri. “He was wearing a patient gown in his social media post, which gave it away since I was wearing the exact same one.”
With a little help from their nurses, a special reunion was quickly planned. Because both are current patients and consistently monitored for any infection that could negatively impact their procedures, including COVID-19, they were able to safely visit with each other.
“We can obviously relate to each other on a lot of different things, and it’s nice to have a support system,” said Queri. “I can rely on him when I have questions or when I’m feeling disappointed. He gets it because he’s been there, too.”
“She went through a big surgery,” said Bartlett, “so we talked about recovery and how we’re both looking forward to getting back home. It was great to see her smiling and feeling better.”
The future of CTEPH treatment
Nearly 2 percent of individuals with first-time pulmonary embolism may develop CTEPH. Until the development of procedures like PTE and BPA, the only treatment available was lung transplantation. Now, UC San Diego Health experts perform approximately 200 PTE procedures and 300 BPA procedures annually and have been training others around the world.
“Our mission is to take care of patients,” said Madani. “As the region’s only academic medical center, it is also part of our mission to educate others and we actively train visiting surgeons to perform this surgery so patients can get the help they need, wherever they are.”
For the 2020-2021 U.S. News & World Report, UC San Diego Health ranked 10 for Pulmonology and 31 for Cardiology and Heart Surgery in the nation’s top 50 programs, out of 4,500 hospitals nationwide.
During the past decade, UC San Diego Health has been consistently rated in the top tier of the Pulmonology specialty, involving medical and surgical therapies for pulmonary (lung) disease. Most recently, UC San Diego Health has led the way regionally in COVID-19 treatment and research. A team of doctors and nurses is collaborating with counterparts in Tijuana and Mexicali to optimize treatment of patients diagnosed with COVID-19 on both sides of the border.
The Cardiovascular Institute at UC San Diego Health offers comprehensive care for advanced heart failure, heart and lung transplantation, complex coronary interventions, heart rhythm disorders, robotic and minimally invasive cardiac surgery, structural and adult congenital heart disease, percutaneous and surgical treatment of thromboembolic pulmonary vascular disease and intensive cardiac rehabilitation.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


