
By:
- Yadira Galindo
Published Date
By:
- Yadira Galindo
Share This:

Dr. Joseph A. Califano III
Telehealth Visits Allow Patients to Connect to Care During COVID-19
A seizure sent Danielle Lovette to the hospital where a brain scan revealed an oligodendroglioma, a cancer of the central nervous system. Subsequent mobility and communications challenges caused by the malignancy, compounded by recovery from necessary surgery and radiation treatments, made the 24-mile round-trips from her home to Moores Cancer Center at UC San Diego Health daunting and exhausting.
With the help of her husband, Corey Nigrelli, Lovette endured the lifesaving treks, but then the novel coronavirus changed everything, including how Lovette attends speech therapy.
“Telehealth video visits have been very helpful,” said Lovette. “Given the current pandemic, they have been the only source of rehabilitation available to me.”
The Numbers
Prior to COVID-19, video visits were used sparingly. UC San Diego Health had completed just 870 telehealth appointments in the preceding three-year period. But days before the state of California issued a stay-at-home ordinance, UC San Diego Health put in motion a plan to provide all of its health care providers with the tools and training they needed to convert in-person appointments to video visits.
In just four days, a team lead by Dr. Christopher Longhurst, chief information officer and associate chief medical officer, Lisa Moore, executive director of the UC Telehealth Collaborative, Dr. Brett C. Meyer, medical director of UC San Diego Health Telehealth, Marc Sylwestrzak, director of Information Services Experience and Digital Health, and Keith Payne, senior director of surgical specialties and hospital affiliations, expedited a large-scale rollout by identifying technology resources on a Thursday, training health care providers and staff on a Sunday and converting more than 1,000 face-to-face clinic appointments to virtual visits by Monday.
Nine weeks into the stay-at-home ordinance, UC San Diego Health has safely increased in-person appointments with health care providers by 26 percent while seeing only a modest 3 percent decrease in video visits. Telehealth visits continue to make up 55 percent of medical appointments.
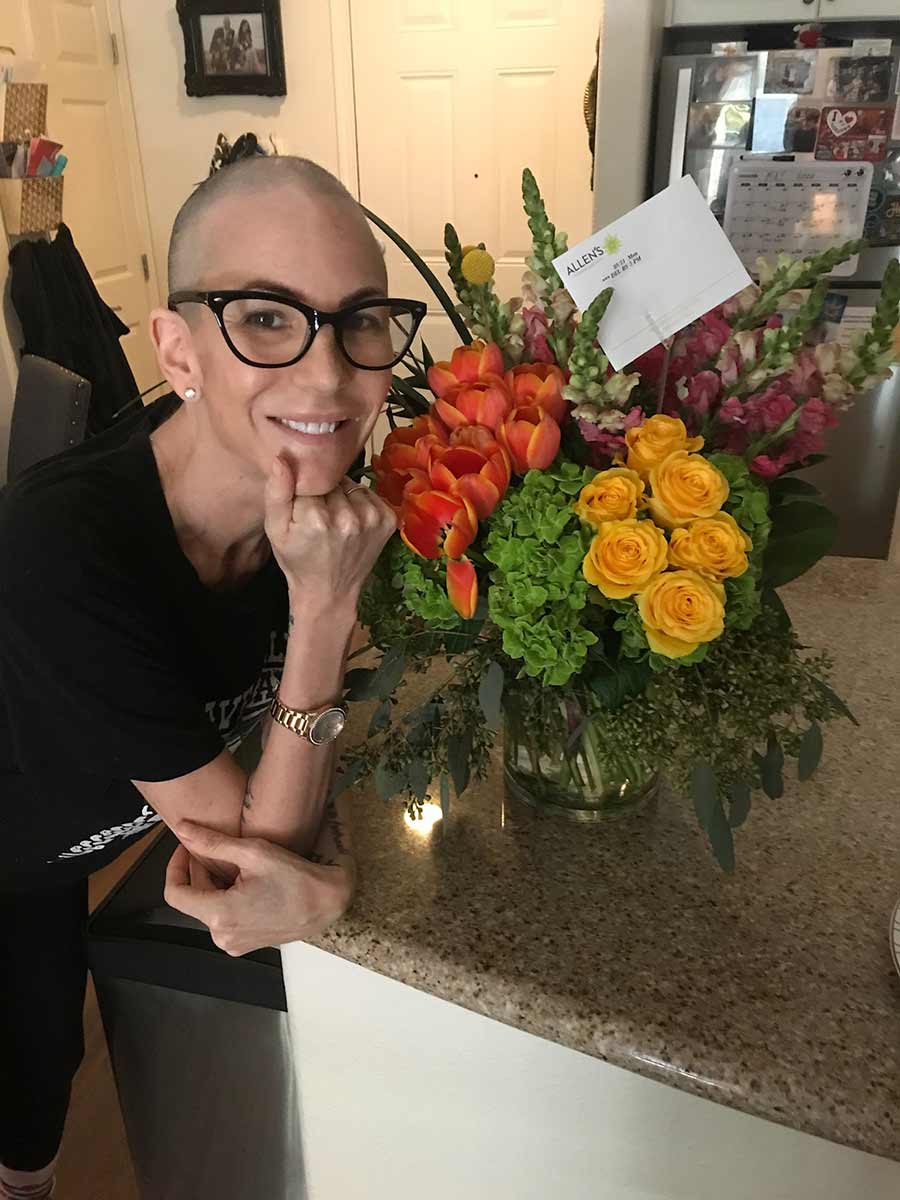
Danielle Lovette
Lovette was among thousands of UC San Diego Health patients who, in the first six weeks of the state’s stay-at-home ordinance, participated in more than 34,000 telehealth visits, allowing them access to essential medical services that range from a consultation with a primary care provider to a post-surgery follow-up appointment.
Once a week, Lovette logs into the MyUCSDHealth app on her mobile device for a live, 45-minute speech therapy video visit. During the session, Liza Blumenfeld, a speech-language pathologist at Moores Cancer Center, might ask Lovette to verbally explain the process of making a sandwich while Lovette is in her kitchen physically preparing it or they talk about Lovette’s dog while she holds it.
“Danielle and I haven’t lost any ground shifting to video visits. In fact, I would say that in her case, telehealth has enhanced functionality because she works at home using words from her day-to-day life,” said Blumenfeld. “We have not cut ties with our patients. We have not allowed COVID-19 to get in the way of providing life-changing care and remaining connected.”
Speech Therapy via Video
Video visits are not ideal for all patients, prompting some providers to get creative, said Blumenfeld, who is currently averaging six telehealth visits per day. People who undergo surgery to remove a tumor from the mouth or throat may need to be re-taught how to eat. Normally, Blumenfeld would see the patient in-person and use sophisticated technology as they swallowed to evaluate progress.
Now, she’ll ask patients to place a penny on the larynx (voice box), which is involved in breathing, talking and swallowing. Seeing the penny rise and fall during swallowing is one indicator of safe swallowing. She can also evaluate voice and speech function. Most importantly, the model allows for patients to receive comprehensive education and support that is essential during cancer treatment.
Currently, 75 percent of appointments at Moores Cancer Center are telehealth visits, said Dr. Joseph A. Califano III, physician-in-chief and director of the Head and Neck Cancer Center at Moores Cancer Center.
“I had a consultation with a patient from Palm Desert who has a tongue cancer and needs surgery. He cannot travel easily so telehealth was a great option for him,” said Califano. “We are able to set up an anesthesia pre-evaluation, schedule surgery, setup pre-op nutrition, speech pathology and survivorship visits. All through telemedicine.”
Telehealth provides people with access to health care services that were previously challenging to access because of location, poor health or the inability to take time off from work, said Califano.
Support services for cancer such as palliative care, speech therapy, psychological services, diet and nutrition are now almost all conducted via telehealth since these visits do not require physical exams, but still help maintain a connection between patients and their health care teams. Moores Cancer Center has also converted many of its support groups and its wellness and education classes to virtual.
“Being in the comfort of my own home and having the ability to sit and conduct face-to-face, personal therapy has been amazing,” said Lovette. “I have enjoyed it so much that I would prefer the telehealth method over the inconvenience of driving to the hospital and conducting the therapy there.”
No Travel
Dr. Howie Tran, UC San Diego Health heart failure and transplant cardiologist, said patients with cardiovascular disease, especially those he sees who have undergone heart transplantation and are taking medications to suppress their immune system, also like that they can visit with their health care team through telehealth while reducing unnecessary public exposures.
Twenty cardiovascular health care providers began using telehealth the first day it rolled out at UC San Diego Health in March. The MyUCSDHealth technology allows patients to consult with multiple providers, from cardiologists to pharmacists to nutritionists—all during the same video visit. An easy-to-follow video explains the process to patients, though departments often call the patients 30 minutes before the appointment time to ensure they can successfully login and fill out any necessary pre-appointment questionnaires.
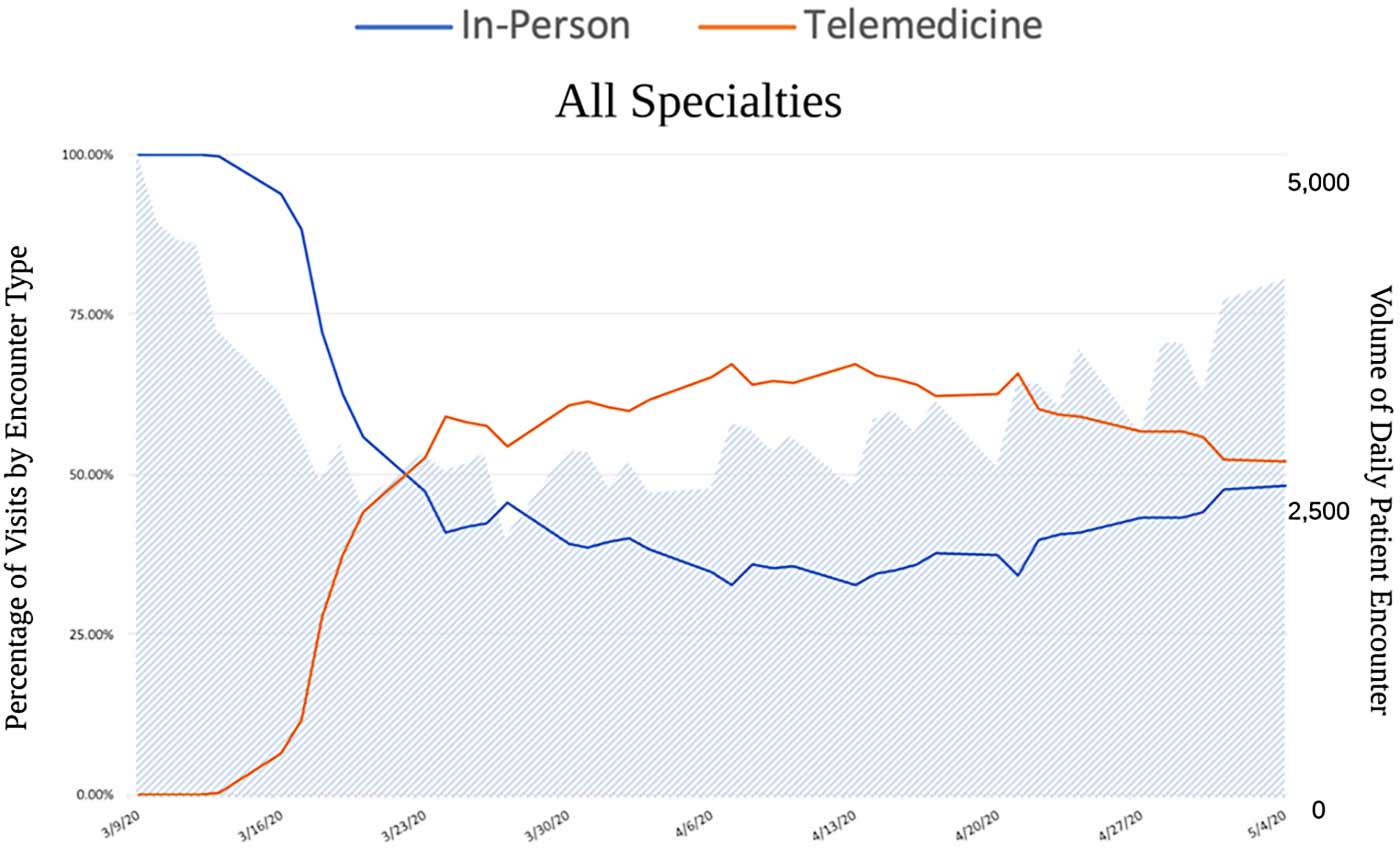
UC San Diego Daily Ambulatory Patient Encounters
While cardiologists prefer to interact with their patients in-person, to listen to their hearts and take other vitals, Tran said there is a place for telehealth even as hospitals transition back to in-person visits. For patients who live outside of San Diego, doing telehealth follow-ups will reduce the stress of travel. On one recent day, Tran had 10 video visits with patients living in Riverside and Orange counties.
If patients are not having active health problems, a video visit can replace some face-to-face appointments, said Tran. Patients with CardioMEMs, an implanted sensor that wirelessly measures heart and lung pressures, can lay down on a specialized pillow to remotely transmit vital information to help aid in crucial management decisions.
“I think telehealth has revolutionized our practice. It is going to change things moving forward,” said Tran. “Even as we return to face-to-face clinics, we will also have telehealth clinics and mobile clinics to accelerate access to appointments. This experience has given us the comfort to resort to telemedicine when necessary, and patients appreciate the flexibility in this practice. We will continue to use virtual visits as appropriate.”
Dr. Jerasimos Ballas, UC San Diego Health maternal-fetal medicine specialist, said his team, which cares for women with high-risk pregnancies, ramped up quickly for the shift to telehealth. Like cardiologists, Ballas said in-person visits with a mother-to-be allows for better evaluation of their well-being and for measuring the fetal heartbeat.
His team conducts new patient visits in-person to understand the patient’s risk and to build a trusting relationship. During that visit, the team will log in with the patient to ensure they are set up on MyUCSDChart and walk them through the process for scheduling future video visits.
“Telehealth has made patients feel safer and that builds trust with us. I would like to continue as least a portion of telehealth visits in the long run such as routine trimester visits. The patients have constant appointments and if telehealth alleviates some of the stress, this can help them,” said Ballas.
Lifesaving Screening
When it comes to eye health, telehealth may make it challenging to diagnose patients. But in one case, Dr. Shira Robbins, an ophthalmologist at Shiley Eye Institute at UC San Diego Health, had no choice. A patient called with new symptoms of double vision but refused an in-person visit because of fears about COVID-19.
“I had a video visit with her that day and diagnosed a new onset sixth nerve palsy, a disorder that causes your eye to cross inward towards your nose. There are many possible causes but because she also had vertigo it concerned me for a significant brain disease,” said Robbins. “I ordered an immediate MRI. The scan revealed a brain aneurysm. We then got the patient to neurosurgery all through telehealth. It can work with the right patient and right set up. I am so glad she called as we likely saved her life.”
Since the COVID-19 pandemic, UC San Diego Health has made telehealth available to all of its providers for clinic appointments, express care services and consultations with patients already hospitalized to help maintain social distancing guidelines. UC San Diego Health has also instituted telehealth services with El Centro Regional Medical Center to provide access to experts without requiring the physical transfer of patients.
Visit the UC San Diego Health website for COVID-19 resources.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


