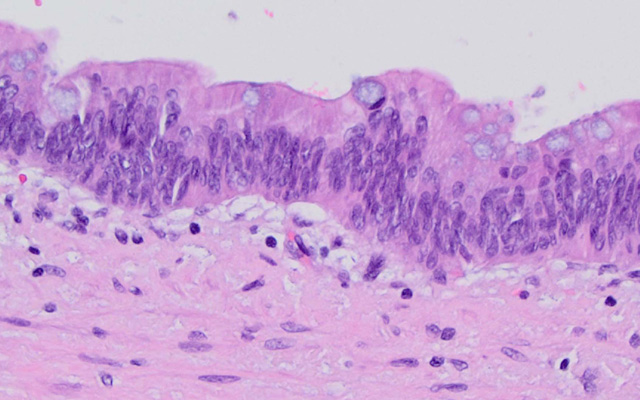
Review of Appendix Cancer Cases Finds Over Diagnosis
Published Date
By:
- Yadira Galindo
Share This:
Article Content
Lesions of the appendix are being over diagnosed as invasive cancer, report University of California San Diego School of Medicine researchers in a paper published June 7 in the journal PLOS ONE.
The scientists found that originating pathologists were more likely to diagnose lesions of the appendix as adenocarcinoma compared to pathologists at a single referral academic medical center. Pathologists with less experience examining tumors of the appendix also had a difficult time diagnosing a tumor of the appendix known as low-grade appendiceal mucinous neoplasm (LAMN).
“Appendix cancer remains extremely challenging for proper pathological classification of tumor type,” said Mark A. Valasek, MD, PhD, assistant professor of pathology at UC San Diego School of Medicine and first author. “This is in part because the appendix can harbor not only invasive cancer, but also an enigmatic and confusing low-grade malignancy called LAMN. In addition, the literature on classification of appendix cancer utilizes inconsistent terminology and is constantly evolving. Our findings highlight a critical need for universally accepted criteria to diagnose appendix tumors to help pathologists separate benign, low grade and invasive tumors.”
Mucinous appendix tumors can lead to pseudomyxoma peritonei, a rare cancer syndrome that most often starts as a lesion in the appendix that bursts, liberating mucus-secreting tumor cells which grow within the abdominal cavity. Properly identifying the type of tumor strongly influences both prognosis and treatment.
Together with researchers from UC San Diego Moores Cancer Center, Valasek and team performed a retrospective pathological chart review to measure agreement between the diagnosis of originating pathologists and a single large academic medical center during patient referral. A search of pathology reports for appendiceal lesions that were first evaluated by an outside pathology group and then referred to UC San Diego Health identified 46 cases over a two-year period.
Originating pathologists identified half of these cases as adenocarcinoma while UC San Diego Health pathologists identified just over one-quarter as such. Originating pathologists diagnosed the other half of the patients with LAMN while UC San Diego Health said 63 percent of patients had LAMN.
In other words, in 57 percent of the cases UC San Diego Health reviewers were in agreement with an invasive cancer diagnosis; overall agreement was 72 percent.
The originating pathologist practices were usually non-academic, mid-sized and did not have subspecialty training in gastrointestinal pathology.
“A second evaluation of appendiceal lesions changed the diagnosis and therefore management of a significant number of patients,” said Andrew M. Lowy, MD, professor of surgery, chief of the Division of Surgical Oncology and senior author. “It is important for someone with expertise in appendix cancer to evaluate pathology reports for the benefit of patients. In addition, recently published guidelines may help facilitate improvement of diagnostic interpretations and reduce over-interpretation and potential overtreatment.”
Co-authors include: Irene Thung, Esha Gollapalle, Alexey A. Hodkoff, Kaitlyn J. Kelly, Joel M. Baumgartner, Vera Vavinskaya, Grace Y. Lin, Ann P. Tipps, and Mojgan V. Hosseini, all at UC San Diego.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.