NIH Awards Researchers $3.1 Million Grant to Improve Treatment of Common Pediatric Heart Condition
Published Date
By:
- Ioana Patringenaru
Share This:
Article Content
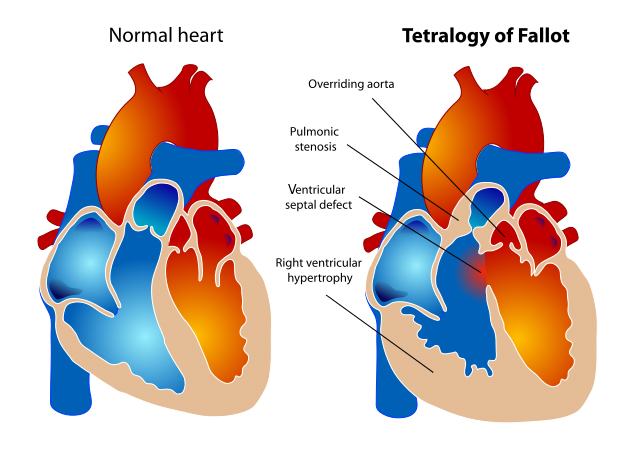
An international team of researchers received a five-year, $3.1 million grant from the National Institutes of Health to discover new and better ways to treat a pediatric congenital heart condition known as tetralogy of Fallot, which affects a total of 85,000 individuals in the United States.
The Cardiac Atlas Project will use machine learning and computational modeling on cardiac imaging data and clinical measurements from 1500 children and young adult patients to develop methods to reduce increased risk of heart failure, electrical rhythm disorders and the need for implanted devices or additional surgical repair procedures.
Specifically, the research team will create a database and develop innovative statistical “atlases” of cardiac shape, biomechanics and electrophysiology to discover new early predictors of clinical outcomes that will help cardiologists better manage patients with tetralogy of Fallot.
“This is an exciting, translational, and international effort," said Dr. James Perry of Rady Children’s Hospital. "Cardiologists are often making decisions on patient care based on less than precise information. This new technology will give us vastly improved understanding of congenital heart structure, physiology, and function. We can then give patients far better predictions of surgical outcomes and give cardiologists better targets for clinical interventions. This will result in restored and preserved cardiac performance over decades for these patients.”
Tetralogy of Fallot is one of the most common congenital heart diseases (or CHD), and makes up about 20% of CHD cases. Patients require surgery before six months of age, often followed by a second intervention during the toddler years.
But these interventions often lead to a condition characterized by a leak in the valve that allows blood to flow back into the heart before reaches the lungs for oxygen. This in turn can lead to an enlarged right ventricle in the heart and can ultimately lead to heart failure. As a result, patient mortality rates triples during their 30s.
Physicians recommend that patients undergo cardiac magnetic resonance exams every three years. The research team plans to use data from these exams to identify biomarkers that could predict long-term side effects from surgery and the potential for heart failure.
The grant is a renewal of the group’s NIH-funded research on congenital heart disease, which affects 1% of live births.
The effort will be led by bioengineers Andrew McCulloch and Jeff Omens at the University of California San Diego, with Dr. Sanjeet Hegde and Dr. James Perry of Rady Children’s Hospital in San Diego and Alistair Young at King’s College London. The grant comes from the National Heart Lung and Blood Institute at the NIH.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.