
For First Time, Scientists Use CRISPR-Cas9 to Target RNA in Live Cells
Technique may open doors to new treatments for many conditions, from cancer to autism
Published Date
By:
- Heather Buschman, PhD
Share This:
Article Content
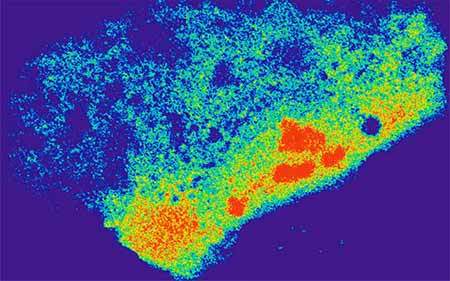
A cell carrying an RNA-targeted Cas9 system that reveals beta-actin mRNA distribution in the cytoplasm.
The genetic code stored in DNA determines everything from the color of our eyes to our susceptibility to disease. This has motivated scientists to sequence the human genome and develop ways to alter the genetic code, but many diseases are linked to a different fundamental molecule: RNA. As the intermediary genetic material that carries the genetic code from the cell’s nucleus, scientists have long sought an efficient method for targeting RNA in living cells. Researchers at University of California, San Diego School of Medicine have now achieved this by applying the popular DNA-editing technique CRISPR-Cas9 to RNA.
The study is published March 17 in Cell.
“This work is the first example, to our knowledge, of targeting RNA in living cells with CRISPR-Cas9,” said senior author Gene Yeo, PhD, associate professor of cellular and molecular medicine. “Our current work focuses on tracking the movement of RNA inside the cell, but future developments could enable researchers to measure other RNA features or advance therapeutic approaches to correct disease-causing RNA behaviors.”
RNA’s location in a cell – and how and when it gets there – can influence whether proteins are produced in the right location and at the appropriate time. For instance, proteins important to neuronal connections in the brain, known as synapses, are produced from RNAs located at these contacts. Defective RNA transport is linked to a host of conditions ranging from autism to cancer and researchers need ways to measure RNA movement in order to develop treatments for these conditions.
Efforts to edit and measure DNA – as a means to alter protein production, study the underlying biology and correct defects to treat disease – got a big boost a few years ago. That’s when researchers discovered they could take CRISPR-Cas9, a naturally occurring defense mechanism bacteria use to fend off invading bacteria, and apply it to edit genes in mammalian systems.
Normally, CRISPR-Cas9 works like this: researchers design a “guide” RNA to match the sequence of a specific target gene. The RNA directs the Cas9 enzyme to the desired spot in the genome, where it cuts the DNA. The cell repairs the DNA break imprecisely, thus inactivating the gene, or researchers replace the section adjacent to the cut with a corrected version of the gene.
Until now, CRISPR-Cas9 could only be used to manipulate DNA. Yeo and colleagues at the University of California, Berkeley, have applied the technique to develop a flexible means of targeting RNA in live cells, also called RNA-targeted Cas9 (RCas9).
In order to target RNA instead of DNA, the researchers altered several features of the CRISPR-Cas9 system. Building upon previous work by co-author Jennifer Doudna, PhD, at UC Berkeley, they designed a short nucleic acid called the PAMmer that, along with the guide RNA, directs Cas9 to an RNA molecule.
To test the system, Yeo’s team targeted the RNA that encodes the proteins ACTB, TFRC and CCNA2. Then they watched as Cas9, fused with a fluorescent protein, revealed the movement of RNA into stress granules, a cluster of proteins and RNAs that form in a cell’s cytosol (the area outside the nucleus) when the cell is under stress. Stress granules are linked to neurodegenerative disorders, such as amyotrophic lateral sclerosis (ALS). This system allowed the team to track RNA over time, in live cells, without the need for artificial tags commonly used in other RNA-tracking techniques – an approach that can interfere with normal cellular processes.
“CRISPR-Cas9 is supporting a revolution in genomics and medicine based on its ability to target and modify human DNA,” said David Nelles, a UC San Diego Jacobs School of Engineering graduate student in Yeo’s lab and first author of the study. “DNA is the fundamental building block of life and we are just beginning to see the implications of genome engineering with CRISPR-Cas9, but many diseases including cancer and autism are linked to problems with another fundamental biological molecule – RNA.”
Study co-authors also include Mark Fang, Jia L. Xu, Sebastian J. Markmiller, UC San Diego; and Mitchell R. O’Connell, UC Berkeley.
This research was funded, in part, by the National Institutes of Health (grants HG004659 and NS075449), California Institute for Regenerative Medicine (grants RB3-05009 and RB4-06045), Howard Hughes Medical Institute, National Health and Medical Research Council of Australia, National Science Foundation Graduate Research Fellowship, Alfred P. Sloan Research Fellowship and Powell-Focht Graduate Fellowship.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


