
Testing Antioxidant Drugs is Transparent
By:
- Debra Kain
Published Date
By:
- Debra Kain
Share This:
Article Content
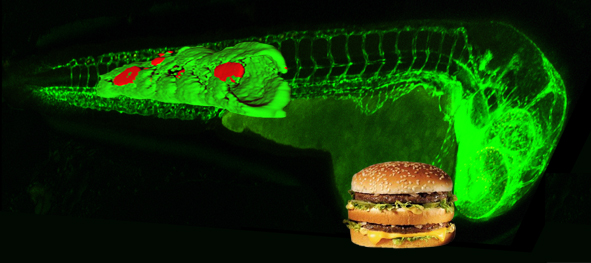
Zebrafish model of atherosclerosis.
A study using genetically modified zebrafish to visualize early events involved in development of human atherosclerosis describes an efficient model – one that the researchers say offers many applications for testing the potential effectiveness of new antioxidant and dietary therapies.
The research, led by scientists from the University of California, San Diego School of Medicine, has been published online by the Journal of Clinical Investigation, and will appear in print in the December 1 issue of the journal.
Atherosclerosis is a process of lipid deposition and inflammation in the artery walls. Low-density lipoprotein (LDL) that carries “bad” cholesterol in blood is easily oxidized, and oxidized LDL promotes inflammatory responses by vascular cells. Inflamed atherosclerotic plaque can often rupture; this results in a blood clot, obstruction of blood flow to the heart or brain, and heart attack or stroke.
An international team of researchers led by Yury Miller, MD, PhD, of the UCSD Department of Medicine, working with colleagues in Australia, developed an approach to see – literally – the accumulation of oxidized LDL in genetically modified zebrafish fed a diet high in cholesterol. Because young zebrafish are transparent, the researchers were able to study vascular lipid accumulation, lipid oxidation, and uptake of oxidized LDL by macrophages – all in live animals.
To be able to see oxidized LDL, the researchers inserted a gene encoding an antibody that recognizes oxidized LDL, conjugated with green fluorescent protein (GFP), into the zebrafish genome. The antibody, called IK17, was originally cloned from a patient with severe coronary heart disease by the group of scientists led by Joseph L. Witztum, MD, and Sotirios Tsimikas, MD, also of the UCSD Department of Medicine.
The new gene was silent in zebrafish until their tank water was warmed to 99ºF (37ºC.) After one hour of this “heat shock,” IK17-GFP was produced and eventually bound to its target – oxidized LDL in the vascular wall. The green glow of GFP was clearly seen in tiny, live zebrafish under microscope. It was then put back into the fish tank until next picture-taking session.
“Using this technique, we were able to measure the time course of oxidized lipid accumulation in the vascular wall and visualize the effects of treatment with an antioxidant drug, and saw that it reversed the accumulation of oxidized LDL,” said the paper’s first author Longhou Fang, PhD. “The same therapeutic effect was achieved by switching the zebrafish back to a diet low in cholesterol. We saw the results in just 10 days working with the zebrafish model. A similar experiment in mice took 6 months to complete.”
“I see this cholesterol-fed, transgenic zebrafish model as a novel way to study early vascular lipid accumulation and lipoprotein oxidation, the processes that lead to heart disease in humans,” said Miller. “Since it is relatively easy and cost-effective to establish and maintain new transgenic zebrafish lines, this offers an in-vivo test for new antioxidants and other drug candidates that could affect development of human atherosclerosis.”
Additional contributors to the study are Simone R. Green, Ji Sun Baek, Sang-Hak Lee, and Elena Deer of UC San Diego Department of Medicine; and Felix Ellett and Graham J. Lieschke of the Walter and Eliza Hall Institute of Medical Research in Melbourne, Australia and the Australian Regenerative Medicine Institute at Monash University.
Funding was provided by the National Institutes of Health, the UC Tobacco-Related Disease Program, the UC San Diego Clinical and Translational Institute and the Leducq Foundation.
Miller and Fang are inventors on patents and patent applications for the potential commercial use of hypercholesterolemic zebrafish, and Witztum and Tsmikas are inventors on patents and patent applications for potential commercial use of antibodies to oxidized LDL, all held by UC San Diego.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


