Scientists Discover a New Signaling Pathway and Design a Novel Drug for Liver Fibrosis
Health & Behavior
By:
Published Date
By:
Share This:

Steffanie Strathdee holds an image of a bacteriophage; her husband, Tom Patterson holds a rendering of A. baumannii, the bacteria that almost killed him.
Bacteriophages are viruses that specifically destroy bacteria. In the early 20th century, researchers experimented with phages as a potential method for treating bacterial infections. But then antibiotics emerged and phages fell out of favor. With the rise of antibiotic-resistant infections, however, researchers have renewed their interest in phage therapy.
UC San Diego School of Medicine has been at the forefront of phage therapy development over the past few years. In March 2016, Tom Patterson, a professor of psychiatry at UC San Diego School of Medicine, became the first known person in the United States to undergo intravenous phage therapy for a multidrug resistant bacterial infection, with emergency approval from the U.S. Food and Drug Administration. He began improving almost immediately, emerging from a months-long coma. After a long recovery, Patterson fully recovered and returned to work.
Since then, seven additional patients with life-threating infections at UC San Diego Health have been treated with experimental phage therapy. To further advance this work, in June 2018 UC San Diego School of Medicine launched the Center for Innovative Phage Applications and Therapeutics (IPATH), the first such center in North America.
Now, for the first time, UC San Diego School of Medicine researchers and their collaborators have successfully applied phage therapy in mice for a condition that’s not considered a classic bacterial infection: alcoholic liver disease.
The study is published in the Nov. 13 issue of the journal Nature.
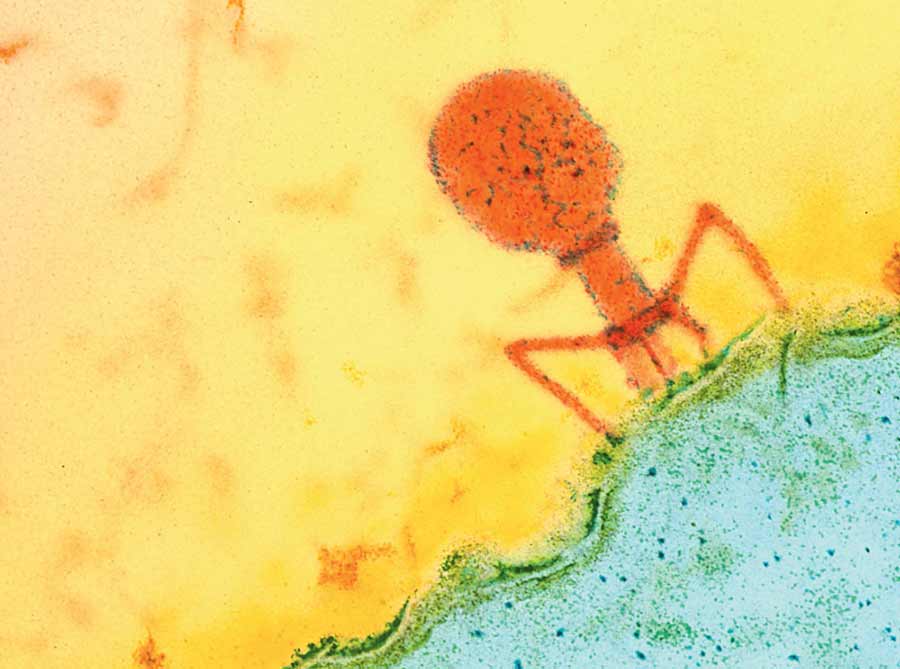
In this false-color micrograph, a bacteriophage (orange) attaches to the membrane of a bacterial cell (blue).
“We not only linked a specific bacterial toxin to worse clinical outcomes in patients with alcoholic liver disease, we found a way to break that link by precisely editing gut microbiota with phages,” said senior author Dr. Bernd Schnabl, a professor of medicine and gastroenterology at UC San Diego School of Medicine and director of the National Institutes of Health-funded San Diego Digestive Diseases Research Center.
Up to 75 percent of patients with severe alcoholic hepatitis, the most serious form of alcohol-related liver disease, die within 90 days of diagnosis. The condition is most commonly treated with corticosteroids, but they aren’t highly effective. Early liver transplantation is the only cure, but is offered only at select medical centers to a limited number of patients. In fact, there are only approximately 8,000 liver transplants for all reasons in the United States each year, according to the American Liver Foundation, with a waiting list of roughly 14,000 people.
Alcohol itself can directly damage liver cells. But Schnabl and team had previously discovered that alcohol is also harmful to the liver for a second reason: It diminishes natural gut antibiotics, leaving mice more prone to bacterial growth in the liver and exacerbating alcohol-induced liver disease.
In this latest study, Schnabl’s team—including many collaborators around the world—addressed two primary questions: How do gut bacteria contribute to liver damage? And can phages be used to reduce the bacteria and thus alleviate alcoholic liver disease?
The researchers discovered that liver cells are injured by cytolysin, a toxin secreted by Enterococcus faecalis, a type of bacteria typically found in low numbers in the healthy human gut. They also found that people with alcoholic hepatitis have more cytolysin-producing E. faecalis in their guts than healthy people. The more E. faecalis present, the more severe their liver disease. For people with alcoholic liver disease, more than five percent of their fecal bacteria were Enterococcus, compared to almost none in healthy people or people with alcoholic use disorder. Approximately 80 percent of alcoholic hepatitis patients have E. faecalis living in their feces, and 30 percent are positive for cytolysin.
Moreover, the researchers found that nearly 90 percent of cytolysin-positive patients with alcoholic hepatitis died within 180 days of hospital admission, compared to approximately 4 percent of cytolysin-negative patients.
“Based on this finding, we believe detection of the cytolysin-gene in feces from patients with alcoholic hepatitis could be a very good biomarker for liver disease severity and risk of death,” Schnabl said. “One day we might be able to select patients for tailored therapies based on their cytolysin status.”
Next the team transferred feces from cytolysin-positive and cytolysin-negative people with alcoholic hepatitis to mice. Mice with cytolysin-positive humanized gut microbiomes developed more severe alcohol-induced liver disease and survived less than mice without cytolysin.
To investigate the potential for phage therapy, the researchers isolated from sewage water four different phages that specifically target cytolysin-producing E. faecalis. When they treated the mice with the targeting phages, the bacteria were eradicated and alcohol-induced liver disease was abolished. Control phages that target other bacteria or non-cytolytic E. faecalis had no effect.
“This phage therapy has only so far been tested in mice, and a clinical trial will be required to test the safety of this approach, and validate our findings in patients with alcoholic hepatitis,” Schnabl said.
Share This:
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.