
By:
- Michelle Brubaker
Published Date
By:
- Michelle Brubaker
Share This:
Program for High-Risk Seniors Offers Dose of Hope During Pandemic
UC San Diego Health’s Population Health Services Organization helps senior patients navigate the COVID-19 vaccination process
Sitting in a wheelchair inside her modest Logan Heights home, Brenda Tanoi, 68, reflects on how the COVID-19 pandemic has impacted her family over the past year. It is a tale of tragedies.
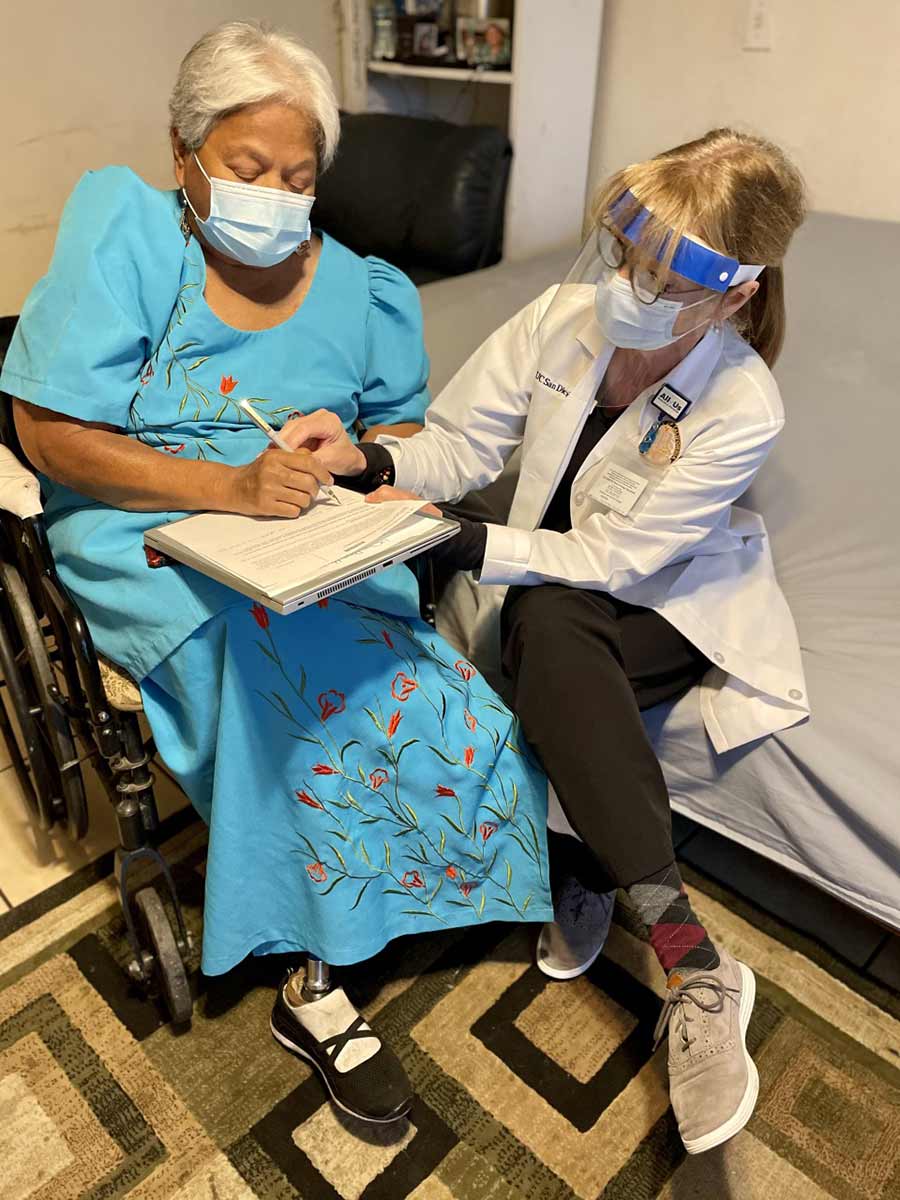
Janet Davis, a nurse-practitioner with UC San Diego Health’s Population Health Services Organization, sits next to Brenda Tanoi, age 68, to go over paperwork before administering Tanoi's second dose of the COVID-19 vaccination from the comfort of her home.
“Since February 2020, I have lost one to two family members or friends each month to this horrific virus, including my son,” said Tanoi. “It has caused a lot of hurt and pain and has left many communities financially drained and facing significant difficulties trying to meet basic necessities.”
Tanoi, a retired educator from American Samoa, was infected with COVID-19 in December 2020. She survived, but some of the symptoms and consequences persist.
After the virus invaded the corneas of her eyes, she lost most of her vision. She suffers from a condition known as “COVID toes,” which can be caused by inflammation in blood vessels or clotting in response to the virus. The impaired circulation renders the toes reddish-purple in color, tender and often with itchy bumps.
For Tanoi, it also means one of her toes may need to be amputated. “I’m willing to lose a toe so I don’t lose a leg or my life.”
On this day in mid-March, Tanoi is home, awaiting a visit by Janet Davis, a nurse-practitioner with UC San Diego Health’s Population Health Services Organization (PHSO), who will provide Tanoi with her second shot of the Moderna vaccine and an extra dose of hope.
“How are you doing today, Brenda?” asks Davis.
“I’m ready for this,” says Tanoi. “There is a lot of vaccine hesitancy in my community, and I am hoping by getting it, I can show my family, friends and neighbors that it is safe and necessary.”
Davis sits next to Tanoi, going over the paperwork, kindly and patiently reading each word and gently guiding Tanoi’s hand on where to sign. Davis asks Tanoi if she had side effects after the first dose.
“Oh yes, I didn’t feel that well,” said Tanoi.
Davis cautions Tanoi on the possible and common side effects from the second dose, how they may be stronger than the first and how to best address any issues that arise.
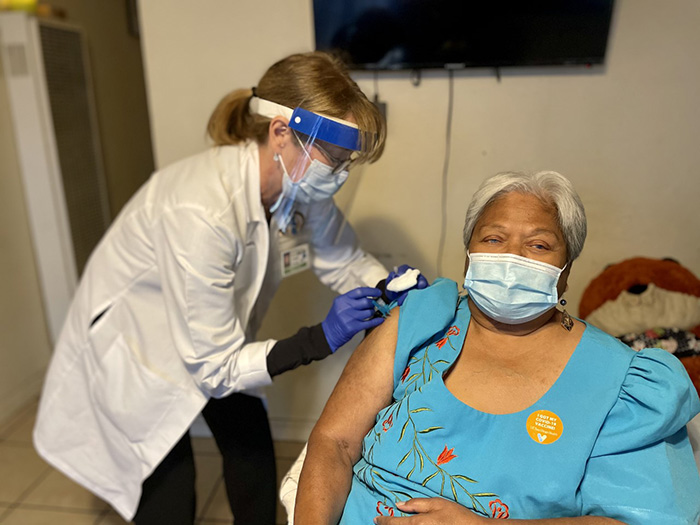
Brenda Tanoi, a retired educator from American Samoa, receives her second dose of the Moderna vaccination through UC San Diego Health's Population Health Services Organization's in-home services for high-risk seniors not able to travel to a vaccination site.
Even with that information and through a mask, Tanoi’s smile shines through. She is seconds away from being even more protected from a virus that has already taken so much.
Phone connections
Fifteen miles away from Tanoi’s home, Matt Finley sits in a call center answering questions, triaging needs, providing vaccine education and sometimes just offering a compassionate ear to callers: UC San Diego Health high-risk patients age 65 and older.
Finley, a UC San Diego Health nursing student, is part of the PHSO team that assists seniors through the vaccination process, from setting up their electronic medical record to scheduling vaccination appointments.
“For some seniors, the technology is complicated, so we are here to help them navigate through it,” says Finley.
High-risk senior patients at UC San Diego Health receive an automated call or text message about the COVID-19 vaccine. Approximately 3,000 calls go out daily. Patients are guided through options. Depending on how a patient responds to the options and questions during that call or text message, they may be transferred to Finley’s team for additional guidance and instructions.
Approximately 20 percent of senior patients contacted by automated call or text are transferred to the call center.
“We address several areas, like vaccine choices and hesitancy,” said Finley. “If they are feeling hesitant, we find out why. Sometimes by the end of the conversation, they want to schedule a vaccine appointment. We make sure if they received their first dose, that they are able to schedule their second.”
The call center collaborates with a PHSO care navigation team who can directly make the vaccine appointments for the senior patients.

Matt Finley (third from left in second row) and the call center team with UC San Diego Health's Population Health Services Organization assist senior patients over the phone, answering questions, triaging a variety of needs and providing COVID-19 vaccination information.
Early in the pandemic, the PHSO sprang into action, bringing together departments, such as social work, nursing and pharmacy, to address the anticipated physical and emotional needs of this vulnerable patient population.
“The vaccine efforts are really an extension of the work already developed in the beginning days of the pandemic,” said Dr. Parag Agnihotri, chief medical officer at PHSO. “We knew there was a critical need in certain populations, such as high-risk seniors. We wanted to create a system that provides evidence-based information and to be there to address all concerns.”
Finley handles 10 to 15 calls daily. There are 10 team members working the phone lines.
“We created a workflow that has evolved with the pandemic through active learning. We joked about building a plane while learning to fly at the same time. We have learned how to be open-minded and flexible with ideas and improvements,” said Ming Tai-Seale, director of research and learning at PHSO. “We try to make doing the right thing the easy thing for our elderly patients, helping them get through the last mile of this marathon.”
Each member in the call center follows a script, which serves as an interview guide, although sometimes the job requires more than just following words on paper.
“I really like connecting with people. It’s the main reason I decided to become a nurse,” said Finley. “This has been a rewarding experience. It feels good when you get off the phone and you know you have helped someone. The goal is to assist in getting as many people vaccinated and protected from this virus as possible. For some of our patients, that means getting their lives back. It means hugging their grandchildren.”
The comfort of home and brighter days
The services provided by PHSO also include in-home vaccinations for seniors who are not able to travel to a site.
“Due to health reasons, some of our patients are confined at home. We want to meet patients where they are,” says Eileen Haley, a registered nurse who serves as PHSO director. “Our efforts are multi-pronged, but serve the same purpose—to get the vaccine in the arms of our high-risk seniors in the community.”
The at-home service was up and running before the pandemic, addressing the health needs of qualifying seniors, but it has taken center stage during COVID-19 vaccinations. Since its inception more than a year ago, there have been approximately 1,000 home visits, involving a coordinated effort between the patient’s primary care physician and visiting nurse-practitioners.
“It’s about building our patients’ confidence and providing excellent health care,” says Victoria Harris, assistant director, clinical quality performance for PHSO.
Back at Tanoi’s home, she is flushed with relief after receiving her second vaccine dose. “This is a step toward brighter days. I am so grateful that UC San Diego Health has worked so diligently to provide extensive outreach in the southeast communities.”
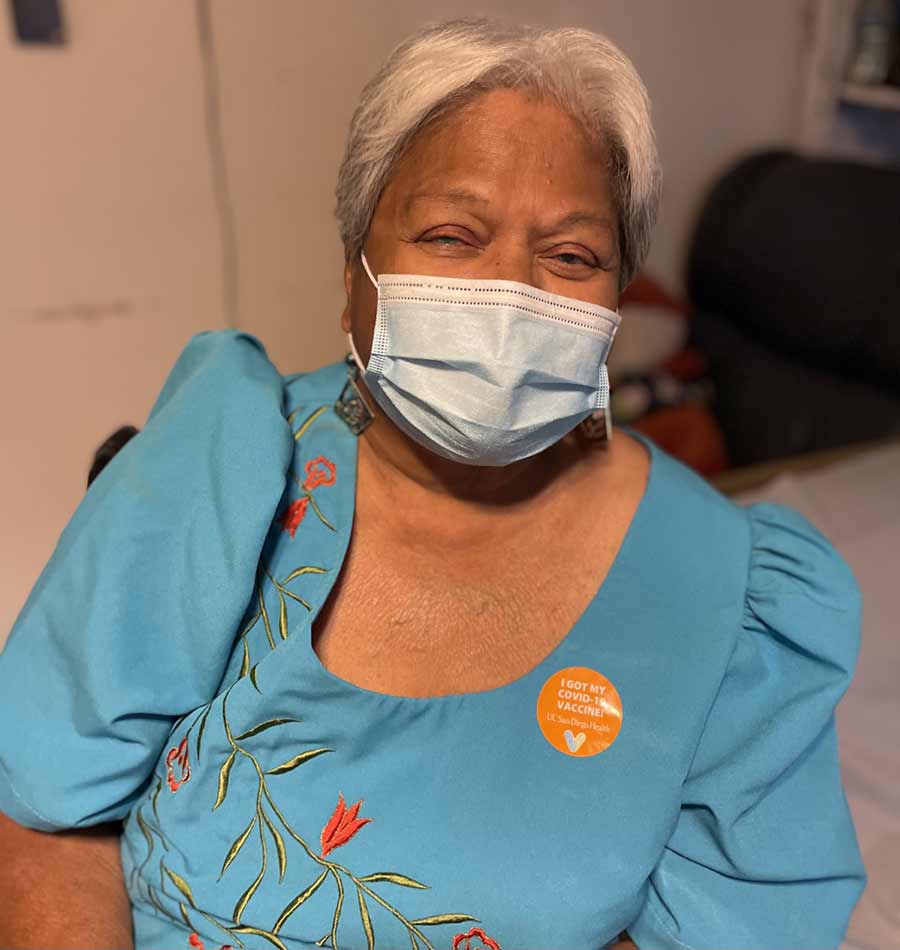
Brenda Tanoi hopes by getting the COVID-19 vaccine she can show her family, friends and neighbors in Logan Heights that it is safe and motivate those who may have vaccine hesitancy to get vaccinated.
Davis, the nurse-practitioner, nods. “The patients are so excited to get the vaccine. We have received positive feedback and sweet notes with messages of gratitude.”
Surrounded by large, family photographs lining her walls, Tanoi takes in the moment.
“It’s been a long road. This vaccine provides some optimism. After all that my family has been through, I am passionate about sharing my story. Getting the vaccine is my way of letting my loved ones know I love them. I want others to be inspired and motivated to also get vaccinated. It will save lives.”
Since receiving her second vaccination, Tanoi has undergone a surgery that has helped to restore her vision, and provide a new perspective.
“I am living more fully now, and I am honored to tell everyone I am fully vaccinated. I want to stop going to memorial services. I want to enjoy many more birthdays and holidays with my family, for as long as I can.”
Learn more about COVID-19 vaccinations at UC San Diego Health.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


